Food Safety
G12 Antibody - Frequently Asked Questions
What peptide sequence does the G12 antibody recognize?
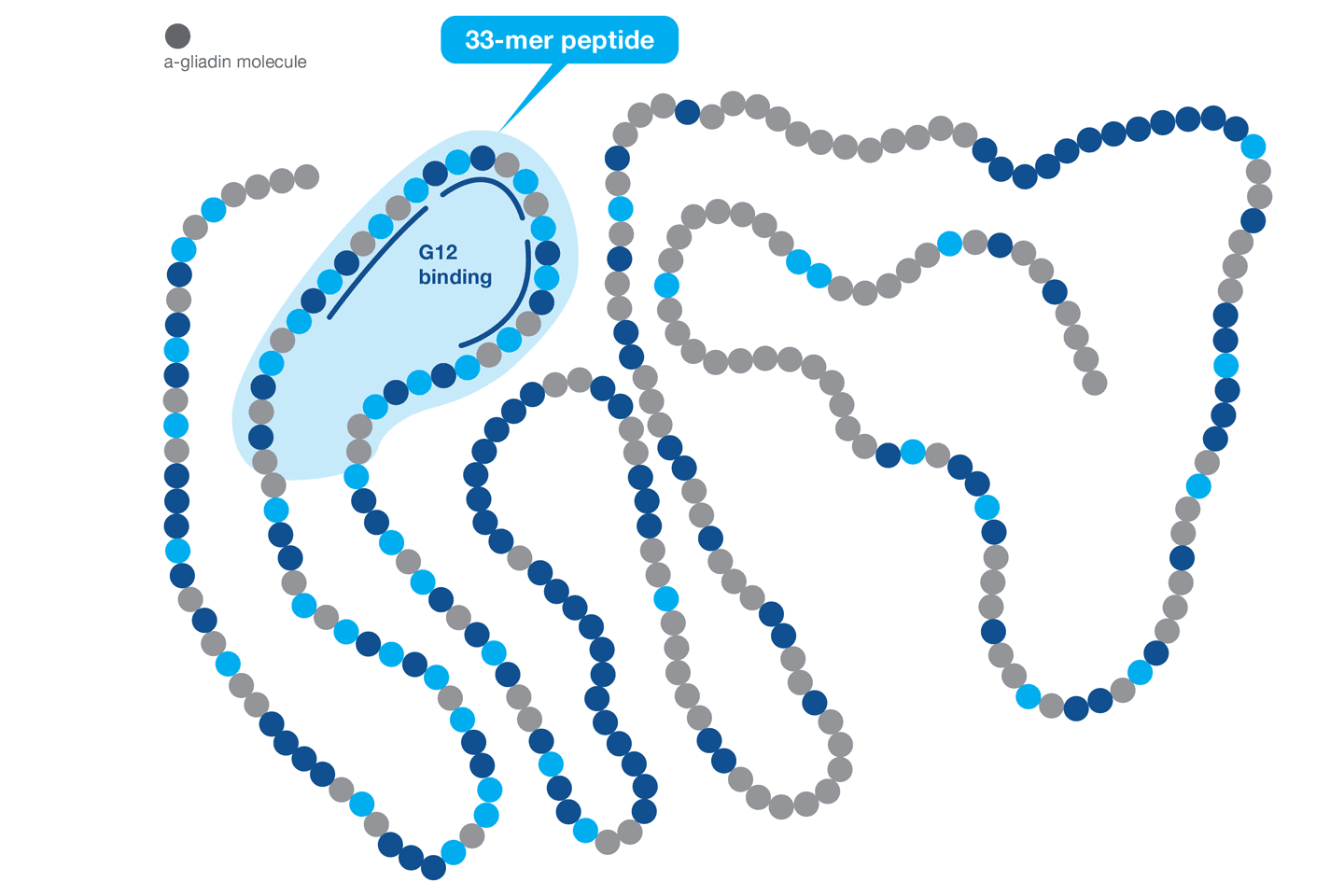
The G12 antibody was raised against the highly immunotoxic 33-mer peptide of the α-gliadin protein that induces celiac disease (Morón et al., 2008). More specifically, the region of recognition within the 33-mer is the hexameric epitope QPQLPY. This recognition sequence is repeated three times within the gliadin 33-mer peptide. The G12 antibody recognizes immunotoxic prolamins from wheat, barley, rye and also from some varieties of oat (Morón et al., 2008). The G12 antibody is also capable of reacting to other epitopes that are found in other toxic prolamins as QPQLPF, QPQLPL, QPQQPY, QPQQPF (Morón et al. 2008; and Real et al. 2014).
Is the G12 antibody reactive to only the 33-mer of the α-gliadin?
No it isn't. The G12 antibody can react to similar sequences present in other gliadins (omega, alfa, gamma and beta) and also in glutenins. The recognition profile of G12 has been largely characterized. (Morón et al., 2008a, Morón et al., 2008b, Real et al., 2014). There are other peptides that could be reactive to G12 that are found in immunogenic peptides of wheat, barley and rye: QPQLPY, QPQQPY, QPQQPF, QPQLPF, QPQLPL, QPELPY.
Is G12 able to detect gluten in beers and other hydrolyzed material?
In hydrolyzed materials such as beers, the relative proportion of reactive peptides for celiac patients may differ, because of the diversity of the resulting peptide populations after fermentation. In a publication a few years ago (Comino et al., 2012), a wide variety of beers were analyzed with two different methods based on the G12 antibody (Competitive ELISA and lateral flow immunoassay) with similar results. Later (Real et al., 2014) a beer legally labeled as gluten-free (undetectable level of gluten by Competitive ELISA R5) was shown to contain gluten peptides determined by ELISA G12 and by Mass spectrometry, which identified immunotoxic peptides for celiac patients. This was shown by exposing cells of the immune system of celiac patients to these peptides and measuring their response. A more recent study (Picariello et al., 2015) analyzed samples of WeissbIer (wheat beer) and detected immunotoxic epitopes with G12. They analyzed these beers with sera of celiac patients as a source of anti-gliadin antibody, confirming that the wheat beer contained peptides with reactivity with sera from celiac patients.
There are more than 1000 gluten peptides know as immunogenic. Does G12 recognize all of them?
Detecting all these peptides with a single antibody is almost impossible. However, a recent study (Moreno et al., 2016) has shown that the most immunogenic peptides (responsible for 80-95% of immunoreactivity of celiac T cells) reacted to G12. In contrast, a widely used antibody in gluten detection, R5, only recognized around 25% of these immunogenic peptides of a barley beer. The correlation between G12 reactivity and T cell immunogenicity has been largely studied in several difficult-to-analyze foodstuffs, such as pure oat varieties or barley varieties (Comino et al., 2011, Comino et al., 2012).
Are oats safe for celiac patients? Are they really gluten-free?
Oats are often subject to cross-contamination (in the field and/or during the manufacturing process). However, even if the oat has been grown and processed carefully, this does not mean that it is always considered a gluten-free food. A study from the year 2011 (Comino et al., 2011) showed that not all oats are equal in gluten immunogenic peptide content. All varieties of oats contain avenin, but each one with a different sequence and structure, and only some of these varieties could be a risk for celiac patients. The gluten from the oat varieties were exposed to cells from celiac patients, and the cells responded appropriately; they only reacted to the potential immunotoxic oat varieties. Therefore, the G12 antibody is the best choice for any company that works with gluten-free oats. Other studies (Real et al., 2012; Comino et al,.2016, Silano et al., 2013) have further characterized the differences of these oats and their immunogenicity. In any case, the wheat gluten always contained at least 40-fold more reactivity to G12 than the most reactive oat variety. Maybe, only the most sensitive celiac patients can be affected by the most reactive oat varieties. Future studies will clarify the threshold level of oats with gluten immunogenic peptides to impact on celiac health.
A celiac patient is following a gluten-free diet. Is there an easy way to know if they are doing it correctly?
Until recently, the only way of assessing the adherence to a gluten-free diet was a biopsy, which is expensive, invasive and disgusting, or a serological test, which, according to several studies, is not accurate enough (Kaukinen et al., 2002; Tursi et al., 2003; Moreno et al., 2015; Comino et al., 2016) and can often lead to false positives or negatives. When gluten is ingested and reaches the gastrointestinal tract it is broken down into smaller pieces, called peptides and ultimately, into amino acids. Some of these peptides (such as the 33-mer) are resistant to this digestion and remain intact. They pass the mucosal barrier and, in celiac patients, trigger the celiac response. These peptides will then be excreted both in urine and feces and their detection in these two kinds of samples is direct evidence of gluten ingestion. A recent study that involved 188 celiac patients showed that around 40% had detectable levels of gluten peptides in their feces. This study used G12 antibody from Hygiena to detect gluten peptides.
- “Diversity in oat potential immunogenicity: basis for the selection of oat varieties with no toxicity in coeliac disease”. Comino I, Real A, de Lorenzo L, Cornell H, López-Casado MÁ, Barro F, Lorite P, Torres MI, CebollaA, Sousa C. Gut 2011 Jul;60(7):915-22.
- “Molecular and immunological characterization of gluten proteins isolated from oat cultivars that differ in toxicity for celiac disease”. Real A, Comino I, de Lorenzo L, Merchán F, Gil-Humanes J, Giménez MJ, López-Casado MÁ, Torres MI, Cebolla Á, Sousa C, Barro F, Pistón F. PLoS One 2012;7(12):e48365.
- “Identification and molecular characterization of oat peptides implicated on coeliac immune response”. Comino I, Bernardo D, Bancel E, de Lourdes Moreno M, Sánchez B, Barro F, Šuligoj T, Ciclitira PJ,Cebolla Á, Knight SC, Branlard G, Sousa C. Food Nutr Res. 2016 Feb 5;60:30324.
- “Sensitive detection of cereal fractions that are toxic to celiac disease patients by using monoclonal antibodies to a main immunogenic wheat peptide”. Morón B, Cebolla A, Manyani H, Alvarez-Maqueda M, Megías M, Thomas Mdel C, López MC, Sousa C. Food Nutr Res. 2008 Feb;87(2):405-14.
- “Toward the assessment of food toxicity for celiac patients: characterization of monoclonal antibodies to a main immunogenic gluten peptide”. Morón B, Bethune MT, Comino I, Manyani H, Ferragud M, López MC, Cebolla A, Khosla C, Sousa C. PLoS One. 2008 May 28;3(5):e2294. doi: 10.1371.
- “Significant differences in coeliac immunotoxicity of barley varieties”. Comino I, Real A, Gil-Humanes J, Pistón F, de Lorenzo L, Moreno Mde L, López-Casado MÁ, Lorite P, Cebolla A, Torres MI, Barro F, Sousa C. Mol Nutr Food Res. 2012 Nov;56(11):1697-707.